How Psychological Stress Worsens Skin Inflammation
How Psychological Stress Worsens Skin Inflammation: The Sympathetic–Eosinophil Axis Explained
Introduction
The link between psychological stress and inflammatory skin diseases such as Atopic Dermatitis has long been recognized in clinical settings. Patients frequently report flare-ups during periods of emotional stress, yet the biological mechanisms behind this phenomenon have remained elusive.
A landmark study published in Science (2026) now provides a mechanistic explanation, identifying a previously unknown neuro-immune pathway that directly connects stress signals from the brain to immune activation in the skin.
This discovery introduces the concept of a sympathetic–eosinophil axis, fundamentally reshaping our understanding of stress-induced inflammation.
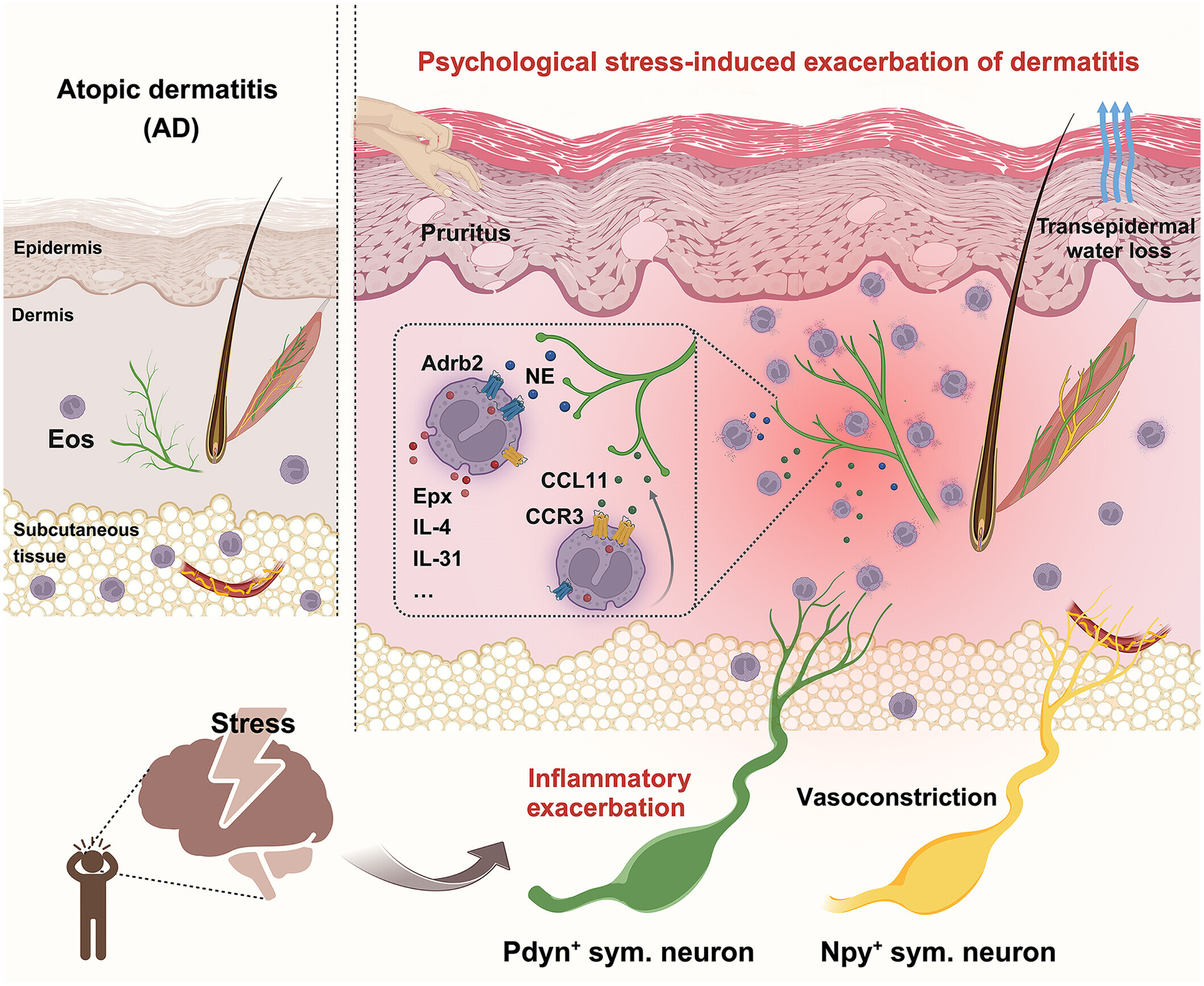
Background: The Skin as a Neuro-Immune Organ
The skin is not only a physical barrier but also a highly dynamic interface between the nervous system and the immune system. It contains:
- Dense networks of sensory and autonomic neurons
- Resident and circulating immune cells
- Rapid-response inflammatory pathways
Among immune cells, Eosinophils play a key role in allergic inflammation and are known contributors to eczema pathology.
However, until now, the direct signaling route from psychological stress to eosinophil activation remained unclear.
Key Discovery: A Brain-to-Skin Signaling Axis
1. Stress Activates Sympathetic Neurons
The study identifies a specialized subset of noradrenergic sympathetic neurons (Pdyn⁺ neurons) that respond to psychological stress.
These neurons:
- Originate in the central nervous system
- Project into peripheral tissues
- Preferentially innervate the skin
This establishes a direct neural communication pathway between emotional stress and skin physiology.
2. Chemokine-Mediated Recruitment of Eosinophils
Upon activation, sympathetic neurons initiate immune signaling via the CCL11–CCR3 chemokine axis.
This leads to:
- Release of chemokines such as CCL11
- Recruitment of eosinophils from circulation into the skin
Result: accumulation of pro-inflammatory immune cells at the site.
3. Adrenergic Activation of Immune Cells
Once in the skin, eosinophils are further activated via:
- β2-adrenergic receptor signaling
This signaling induces:
- Cytokine release
- Amplification of inflammation
- Tissue damage and itching
This step transforms recruited eosinophils into active drivers of disease pathology.
Experimental Evidence
The study combined human clinical observations with advanced animal models, providing strong causal evidence.
Key Results:
- Increased stress levels correlate with:
- Higher eosinophil infiltration
- Increased disease severity
- Selective removal of:
- Sympathetic neurons
- OR eosinophils
Completely abolished stress-induced inflammation
- Artificial activation of neurons:
Exacerbated inflammatory responses
These findings confirm that stress is not merely associated with disease but is a direct biological driver.
Mechanistic Model
The pathway can be summarized as follows:
Psychological Stress → Sympathetic Nervous System Activation → Skin Innervation → Chemokine Release → Eosinophil Recruitment → Adrenergic Activation → Inflammation
This represents a closed neuro-immune loop linking emotional states to immune dysfunction.
Clinical Implications
1. Novel Therapeutic Targets
The study identifies multiple intervention points:
- Sympathetic neuron signaling
- Chemokine pathways (CCL11–CCR3)
- Adrenergic receptors
- Eosinophil activity
These targets open the door to next-generation treatments for inflammatory skin diseases.
2. Redefining Stress in Disease Management
This research demonstrates that stress:
- Is not just a psychological factor
- Directly influences immune responses
- Plays a causal role in disease progression
Integrating stress management into treatment protocols becomes biologically justified, not just supportive care.
3. Broader Impact Beyond Dermatology
The identified neuro-immune mechanism may extend to other conditions:
- Allergic diseases
- Autoimmune disorders
- Chronic inflammatory syndromes
Suggesting a universal principle of neuroimmune regulation.
Scientific Significance
This study represents a major breakthrough in:
- Neuroimmunology
- Dermatology
- Psychosomatic medicine
It provides:
✔ A direct molecular link between brain and immune system
✔ Evidence for neural control of inflammation
✔ A new framework for understanding stress-related diseases
Conclusion
The discovery of the sympathetic–eosinophil axis fundamentally transforms our understanding of how psychological stress affects physical health.
Rather than acting indirectly, stress:
- Activates neural pathways
- Recruits immune cells
- Drives inflammation at the tissue level
This work paves the way for integrated therapeutic strategies combining neurology, immunology, and mental health interventions.
References
- Tian J. et al. (2026). A sympathetic–eosinophil axis orchestrates psychological stress to exacerbate skin inflammation. Science. DOI: 10.1126/science.adv5974
Recent Posts
-
How Psychological Stress Worsens Skin Inflammation
How Psychological Stress Worsens Skin Inflammation: The Sympathetic–Eosinophil Axis Explained Introd …23rd Mar 2026 -
Genomic DNA Extraction Kit
Genomic DNA Extraction Kit: A Comprehensive Scientific Overview Introduction A genomic DNA extractio …23rd Mar 2026 -
Mapping Protein–Protein Interactions by Mass Spectrometry
Mapping Protein–Protein Interactions by Mass Spectrometry: A Comprehensive Guide to Modern Interacto …18th Mar 2026
